Treatments


Lower back pain
Low back pain can be acute (recent onset) or chronic, meaning it has been present for more than a few months.
Acute low back pain can feel sudden, frightening and disabling, often developing during a normal everyday movement. When pain is severe, it is natural to assume something serious has happened, such as a disc injury, joint inflammation or a “slipped” disc.
In the majority of cases, however, low back pain is not caused by structural damage and does not require an X-ray or scan. An osteopath or physiotherapist will assess your condition to determine whether imaging is needed or whether it is safe to begin hands-on treatment and movement therapy.
Although pain can be severe, recovery is often quicker than expected. However, it is important to have realistic expectations, as recovery depends on a combination of physical, psychological and lifestyle factors unique to each individual.
At Alison’s osteopathy clinic in Kensal Rise, West London, all of these factors are considered when developing a personalised treatment plan to support your recovery from low back pain.
Upper back pain
Like low back pain, upper back pain may be acute (recent onset) or chronic. When it develops suddenly, it is often painful and restrictive, although usually less disabling than low back pain.
Because the rib cage and diaphragm attach to the thoracic spine, upper back pain can sometimes be associated with difficulty taking a deep breath or a feeling of restricted breathing.
There are many possible contributors to upper back pain, including posture, shoulder strength and mobility, a tight or tense neck, and the relationship between upper back movement and breathing. Psychological factors such as stress and anxiety can also play an important role.
All contributing factors are carefully assessed to build a clear understanding of your condition. This allows for a tailored treatment approach that supports recovery, improves movement, and helps you manage and resolve symptoms effectively.
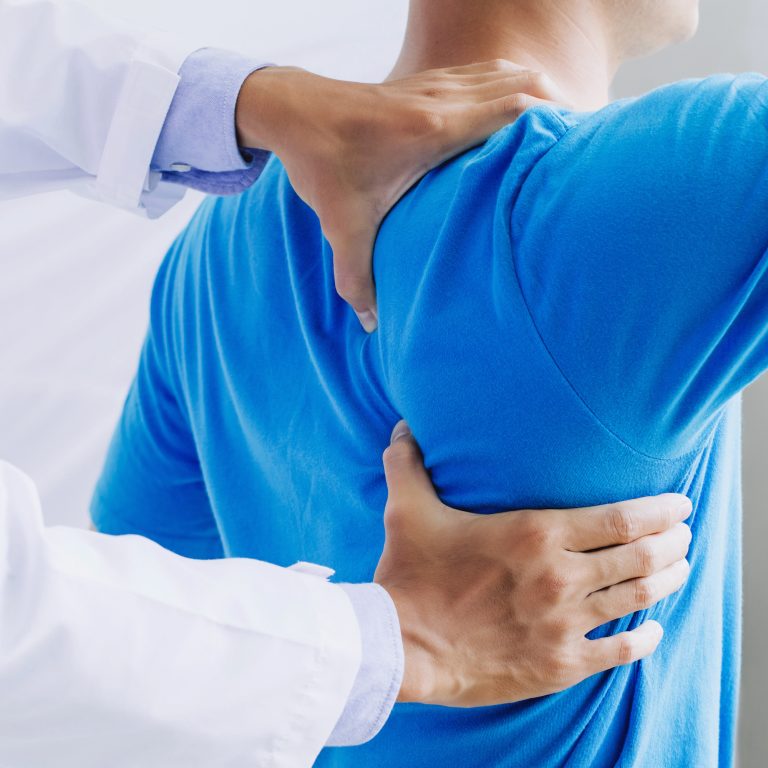



Shoulder pain
Shoulder presentations in commonly include pain, stiffness and reduced range of movement, often affecting daily activities such as reaching, lifting or dressing. These symptoms may arise from local shoulder dysfunction or be influenced by the neck, upper back and surrounding kinetic chain.
Identifying the type of shoulder condition is important, as treatment and rehabilitation will depend on the underlying cause.
Treatment involves not only working directly on the shoulder but also assessing how other areas of the body may be influencing its function. A combination of hands-on osteopathic techniques, movement therapy, and exercise rehabilitation is used to support recovery and restore function.
Tennis elbow (lateral epicondylitis)
The most common elbow presentation is tennis elbow, where the tendons on the outside of the elbow become irritated due to overuse, repetitive strain, or sudden increases in activity.
Despite its name, tennis elbow can affect anyone who performs repetitive or forceful movements of the forearm and wrist.
Assessment focuses not only on the elbow but also on the shoulder and upper back, as reduced strength or mobility in these areas can increase load through the elbow.
Treatment typically includes hands-on osteopathic techniques, specific strengthening exercises, and rehabilitation of both local and contributing areas. Advice may also include activity modification, ergonomic changes, and the use of support such as bracing or taping where appropriate.




Knee pain
Although the knee is primarily a simple hinge joint, it is subject to high levels of stress as it sits between the tibia (shin bone) and femur (thigh bone), acting at the end of two long levers.
Knee pain is common in sport and often emerges when activity levels increase, such as with running, squatting, or returning to exercise after a period of inactivity.
Many patients report stopping sport due to knee pain. However, with the right exercise dosage, strengthening programme, and support from surrounding areas such as the hip, foot and ankle, knee capacity can often be improved significantly.
Treatment focuses on improving load tolerance through targeted exercise, hands-on osteopathic techniques, and addressing contributing factors such as movement patterns, footwear, and, where appropriate, orthotic support.
Hip pain
Hip joint pain can be felt deep in the groin or around the side and back of the pelvis.
The gluteal muscles that act on the hip play a key role in movement and stability, acting as a bridge between the upper and lower body. When they become overloaded or fatigued, they can be a common source of pain and dysfunction.
Symptoms may be localised or referred into the lower back, and can range from a mild ache to more significant pain that affects daily activities.
It is common for patients to worry that the hip joint itself is damaged, but in many cases symptoms are related to the surrounding musculature rather than the joint. A thorough assessment by an osteopath or physiotherapist will help determine the likely source of symptoms and whether further investigation, such as imaging, is required.
Treatment focuses on improving load tolerance and function through hands-on osteopathic techniques, targeted exercise rehabilitation, and addressing contributing factors across the hip, pelvis and lower back.




The Ankle
Tendon issues: The ankle and foot are subject to tendon issues that affect the inside and outside of the ankle and at the heel and lower calf (the Achilles tendon). Tendons often become symptomatic when we increase training but can also start to affect us with no change in our daily or sporting regime.
Tendons become stressed when loads exceed their capacity to manage them. In addition to ensuring that joints and muscles further up the body – hip – trunk are not limiting the tendon’s ability to load optimally, it is generally necessary to strengthen the tendon and muscle it attaches to and modify training regimes.
Ankle sprains: Ankle sprains are amenable to treatment even in the hours and days after injury. It is always a good idea to get an ankle sprain checked out by a physical therapist, as failure to rehabilitate it satisfactorily can mean that instability or subtle residual limitation could cause problems down the line – even many years later.
Wedges and insoles can again be useful adjuncts to treatment, when necessary, for a range of foot, ankle, lower leg and knee presentations.
The Foot
Hallux abductus: Hallux abductus is an adaptation of the forefoot in which the metatarsal on the medial border of the foot deviates medially and the big toe deviates laterally. It is an adaptation in response to forces accumulating at the metatarsophalangeal joint and can be painful and make wearing some footwear difficult.
In its early stages treatment interventions can be useful in stopping it in its tracks. An insole or support (wedge) of some sort will usually be very effective in combination with exercise therapy.
Plantar fasciitis: The plantar fascia on the sole of the foot is like an elastic spring. It gets loaded with potential energy when we roll forward on the foot during walking and running.
The flexibility of our big toe, ankle and calf are important in allowing the elastic spring to load efficiently. Limitations in these joints and others and previous ligament injury around the ankle are usual suspect when the plantar fascia is painful.
Often we need targeted exercises to create greater stability, flexibility and strength. Wedges or insoles can also be useful and are sometimes only needed in the short term to give relief.




Arthritic conditions
Osteoarthritis is a degenerative joint condition involving structural changes such as thinning of cartilage, bony changes at the joint surfaces, and thickening of the joint capsule. These changes develop over time in response to load and stress on the joint.
Treatment approaches focus on improving how the joint is used and supported, rather than simply addressing the joint itself. This involves reducing excessive load by improving the function of the joints above and below, while also building strength locally and across the wider movement system.
Research shows that gradually increasing and appropriately dosing activity can significantly reduce pain and improve function over time, particularly in conditions such as knee osteoarthritis, often within a period of around six months.
The aim is to help you stay active, improve joint tolerance, and manage symptoms effectively through a combination of hands-on treatment, exercise therapy, and movement advice.
Persistent pain
Persistent or chronic pain is generally defined as pain that has continued for more than 12 weeks, even after injury has healed or initial treatment has been provided. In many cases, pain has been present for much longer before patients are able to access appropriate help.
Over time, the nervous system can become more sensitive, changing the way signals are processed between the body, spinal cord, and brain. As a result, pain may persist even when there is no ongoing tissue damage.
A helpful way to understand this is to think of pain as an alarm system. In persistent pain, this system can become over-sensitive and trigger too easily. At the same time, the nervous system’s “filtering” or triage function can become less efficient, allowing more signals through to the brain, resulting in pain, stiffness, or other symptoms.
Treatment focuses on helping to calm and retrain this system through a combination of hands-on care, movement-based therapy, education, and strategies that improve confidence in movement and daily activity.


Read more about pain associated with specific areas of the body in the “Treatments for” section.
You can book an appointment here or if you have any questions you’d like to run by me:


